Today’s topic is all About Beck’s Triad or Cardiac Tamponade Triad in Cardiology: Definition, Components, Pathophysiology, Mnemonic, and Treatment.
Are you looking for trustworthy, detailed information about Cardiac Tamponade Triad or Beck’s Triad in Cardiac Tamponade? This is one of the most popular triads in the medical world.
Whether you are a nurse who is searching for a useful guide about Beck’s triad for USMLE and other exams, or you may be a paramedic, medical personnel, or anybody interested in medical terms, today’s topic is just for you. So, let’s begin.
What is Beck’s Triad or Cardiac Tamponade Triad?
Also known as acute cardiac tamponade triad or heart tamponade triad, Beck’s triad is a collection of three classic cardiovascular signs that indicate cardiac tamponade. Cardiac tamponade is a medical emergency in which the excess fluid accumulated in the pericardial sac impairs the heart’s ability to pump blood.
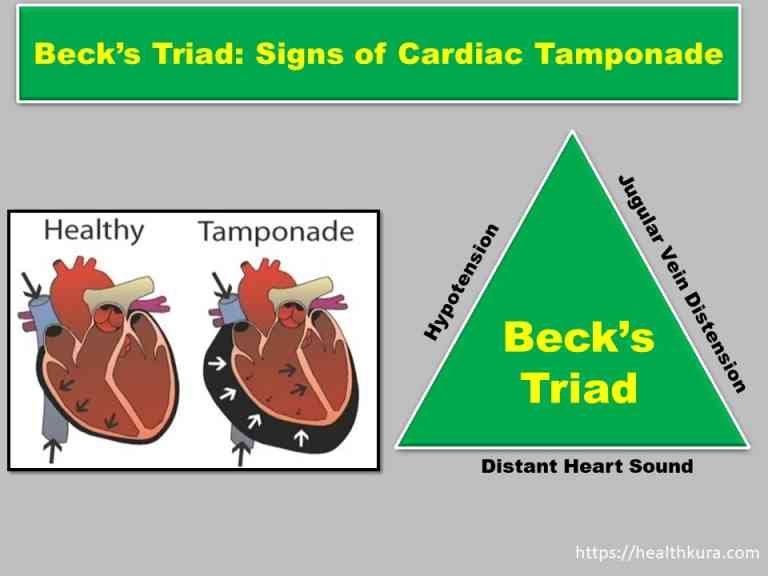
Components of Becks Triad
The classical diagnostic features of cardiac tamponade (components of Beck’s Triad) are:
- Falling blood pressure – Hypotension (weak pulse or narrow pulse pressure)
- Distant or decreased Heart sound (muffled heart sounds)
- Rising jugular venous pressure (distended jugular veins)
Beck actually described two triads, one for acute cardiac tamponade (CT) and another for chronic tamponade.
Beck’s triad for chronic tamponade consists of jugular vein distention(JVD), ascites, and decreased heart sound (muffled heart sounds).
Beck’s triad for acute tamponade consists of jugular vein distention, hypotension, and muffled heart sounds.
Almost 90% of patients of tamponade have at least 1 of the signs, but only one-third have all of the three signs. Furthermore, a late manifestation of cardiac tamponade shows all three signs, usually preceding cardiac arrest.
History and Etymology of Cardiac Tamponade Triad
The terms Beck’s Triad are named after Claude Beck (1894-1971) who first described the concept of this medical triad in 1935. Claude Beck was an American cardiothoracic surgeon and Professor of Cardiovascular Surgery at Case Western Reserve University in Cleveland, Ohio.
What is Cardiac Tamponade?
According to DailyMedEd.com, Cardiac tamponade is a medical emergency that refers to a fluid accumulation around the heart. The collection of this fluid exerts pressure on the heart and decreases the ability of the heart to pump appropriately. As a consequence, there is a collection of three medical signs associated with acute cardiac tamponade, known as Beck’s Triad.
The double-layered pericardium surrounds the heart by the formation of a pericardial sac (filled with about 25 to 50 ml of fluid). The fluid essentially acts as a cushion and allows the heart to contract and expand in a smooth fashion by minimizing friction.
When excess fluid fills the pericardial space, the pericardium is unable to stretch or expand to accommodate the increase in fluid.
If that pressure from the fluid becomes more than the pressure in the heart’s chambers, the heart will begin to compress and lose its natural ability to pump blood to the lungs and circulate blood to the rest of the body.
The signs of acute cardiac tamponade are hypotension, distended neck veins, and muffled heart sounds. The patient will also be complaining of dyspnea and chest pain along with the following signs:
- PE will show muffled heart sounds, JVD and hypotension (Beck’s triad), pulsus paradoxus
- ECG will show low voltage QRS, electrical alterans
- Echocardiography will show the diastolic collapse of RV
Some other symptoms of tamponade that can accompany Beck’s Triad are:
- Tachycardia or a rapid heart rate
- Cold and clammy extremities
- Anxiousness and restlessness
Pathophysiology of Becks Triad

How cardiac tamponade leads to hypotension?
A physiological fall in arterial blood pressure occurs because the heart is hindered in its ability to pump blood. When the heart cannot contract efficiently, the rest of the body does not get supplied with the necessary amount of blood. This can result in the body going into shock and even cardiac arrest.
In short, the inability of the ventricles to contract properly reduces cardiac output resulting in hypotension.
Why does tamponade cause distended jugular veins?
The diastolic filling decreases because of the exerted on the right ventricle. As a result, blood flows back into the right atria and the veins that return blood to the heart, most notably the jugular veins.
In a patient with cardiac tamponade, the rising central venous pressure (jugular vein distension) will be present even when they are sitting upright.
In short, the distention of jugular veins occurs due to the backup of fluid into the jugular veins draining into the heart.
How tamponade leads to distant or decreased cardiac sound?
Muffled heart sounds occur due to the insulating effect of the fluid in the pericardial sac. When sound travels through fluid, it sounds distant or suppressed as it is traveling through a thicker median.
In short, the decreased heart sound occurs because of the muffling effects of the fluid surrounding the heart (pericardium).
The full triad of Beck’s is present only in a minority of cases of acute and chronic tamponade. But if present, the cardiac tamponade triad signals the pathognomonic condition of cardiac tamponade.
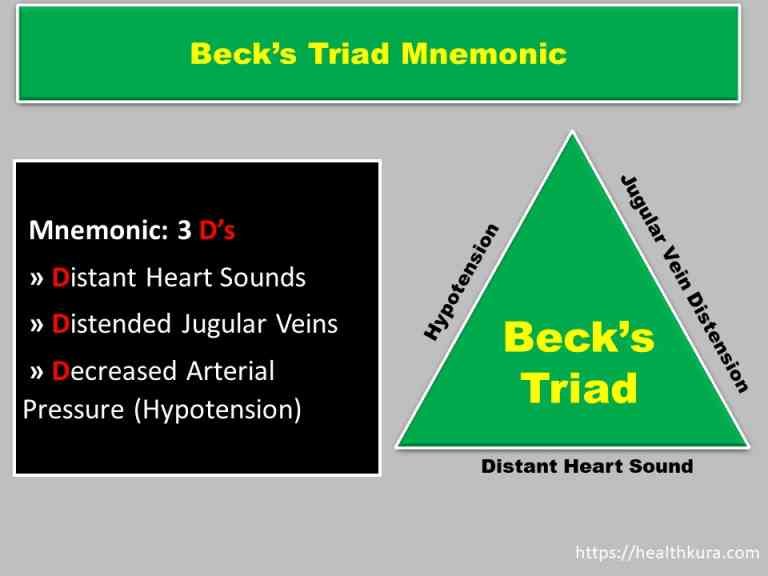
Beck’s Triad Mnemonic (Cardiac tamponade triad mnemonics)
3 D’s
» Distant Heart Sounds
» Distended Jugular Veins
» Decreased Arterial Pressure (Hypotension)
Beck’s Cognitive Triad for Depression
Some people might get confused about Beck’s Triad for Beck’s Cognitive triad of Depression. But it is a completely different condition that is associated with psychology and psychiatry. Also known as a negative triad, Beck’s cognitive triad is a cognitive-therapeutic view of the three key elements of a person’s belief system present in depression.
It was proposed by Aaron Beck in 1976. The triad forms part of his cognitive theory of depression and the concept is used as part of Cognitive Behavioral Therapy (CBT), particularly in Beck’s “Treatment of Negative Automatic Thoughts” (TNAT) approach.
Beck’s Triad vs Cushing’s Triad
Beck’s triad is a characteristic feature of cardiac tamponade in cardiology whereas Cushing’s triad is seen in increased intracranial pressure or ICP. Similarly, Distant Heart Sounds, Distended Jugular Veins, and Decreased Arterial Pressure (Hypotension) (3Ds) are hallmarks of becks triad. But, bradypnea, systolic hypertension, and bradycardia are the characteristic features of the Cushings triad.

YOU MAY ALSO LIKE: Hot Potato Voice or Speech in Peritonsillar Abscess
Treatment of Cardiac Tamponade with Beck’s Triad
As it is a medical emergency, a patient with a cardiac tamponade triad needs immediate hospitalization. There is no intervention you can do pre-hospital for the patient. The doctor will treat the patient to relieve pressure on your heart and then treat the underlying condition. Initial treatment involves your doctor making sure you’re stabilized.
Your doctor will use a needle to drain the fluid from your pericardial sac. This procedure is called pericardiocentesis. Your doctor may perform a more invasive procedure called a thoracotomy to drain blood or remove blood clots if you have a penetrating wound. There might be a condition to remove part of your pericardium to help relieve pressure on your heart.
Let’s summarize Beck’s triad in cardiac tamponade with the following question:
Question 1
Which of the given options best describes Beck’s Triad?
Answer Choices
- Hypertension, JVD, muffled heart sounds
- Hypotension, JVD, muffled heart sounds
- Hypertension, bradycardia, irregular breathing
- Fever, Pain, Jaundice
Explanation
The Correct Answer is B – Hypotension, JVD, and muffled heart sounds.
Answer A – is incorrect. Cardiac Tamponade Triad includes hypotension, not hypertension.
Answer C – is incorrect. It describes Cushing’s Triad in pt. with increased intracranial pressure in cases such as traumatic intracranial hemorrhage from trauma.
Answer D – is incorrect. It describes Charcot’s Triad in pt. with ascending cholangitis
Sources
- Ogilvy, CS; Dubois AB (1987). “Effect of increased intracranial pressure on blood pressure, heart rate, respiration and catecholamine levels in neonatal and adult rabbits”. Biology of the Neonate. 52 (6): 327–336. doi:10.1159/000242728. PMID 3435736.
- Ayling, J (2002). “Managing head injuries”. Emergency Medical Services. 31 (8): 42. PMID 12224233.
- Cushing, H (1901). “Concerning a definite regulatory mechanism of the vasomotor centre which controls blood pressure during cerebral compression”. Bull Johns Hopkins Hosp. 12: 290–2.
- Caroline, Nancy (2013). Emergency Care in the Streets (7th ed.). Jones and Bartlett Learning. p. 1665. ISBN 978-1-4496-4151-1.
- Early management of severe traumatic brain injury. Rosenfeld JV, Maas AI, Bragge P, Morganti-Kossmann MC, Manley GT, Gruen RL Lancet. 2012 Sep 22; 380(9847):1088-98. [PubMed]
- https://codehealth.co/case/376
- Harper RJ. Pericardiocentesis. In Clinical Procedures in Emergency Medicine, 5th ed. Roberts JR, Hedges JR, et al. eds. Saunders, Philadelphia, 2010.
- https://medlineplus.gov/ency/article/000194.htm
- https://www.roshreview.com/blog/teaching-image-cardiac-tamponade/
- Chaiwat O, Sharma D, Udomphorn Y, Armstead WM, Vavilala MS J Neurotrauma. 2009 May; 26(5):657-63. [PubMed]
YOU MAY ALSO LIKE
Rings in Eyes (Ophthalmology): Cholesterol, Blue, & More
Carpal Bones Mnemonic: Wrist Bones Names in Order
Cushing’s Triad in ICP: Pathophysiology, Mnemonic, & More
Acronym for Cranial Nerves Mnemonic – Dirty, Funny Tricks